Understanding TSH Levels: Normal Ranges Explained


Intro
Understanding thyroid function is vital to maintaining overall health. The thyroid-stimulating hormone, commonly referred to as TSH, is a key player in this delicate balance. Fluctuations in TSH levels can reveal a lot about one’s health, providing insights into metabolism, energy levels, and even mood. As we dig into the normal range of TSH, it’s crucial to comprehend how this hormone operates, the factors influencing its levels, and what abnormal results can indicate.
Background and Context
Overview of the Research Topic
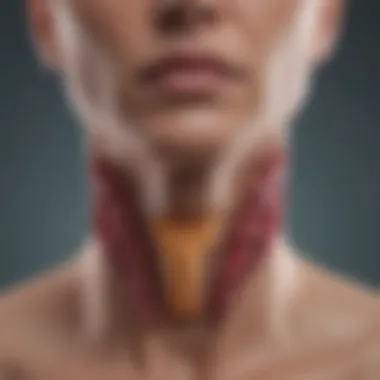
The thyroid gland, nestled at the base of the neck, is small but mighty. It produces hormones that significantly influence your body's metabolism. TSH, synthesized by the pituitary gland, instructs the thyroid on how much thyroxine (T4) and triiodothyronine (T3) to produce. Monitoring TSH levels offers a glimpse into thyroid health and metabolic efficiency. While normal TSH levels range roughly from 0.4 to 4.0 mIU/L, these can vary based on numerous factors, including age, gender, and even the time of day.
Historical Significance
Understanding TSH's role and its normal range is not a recent phenomenon. It traces back to the mid-1900s when advancements in endocrinology began unraveling the intricate relationships between different hormones. Early studies highlighted the implications of abnormal TSH levels, illuminating connections to conditions like hypothyroidism and hyperthyroidism. Over the decades, researchers have fine-tuned TSH reference ranges, taking into account advancements in technology and a deeper understanding of thyroid physiology.
Key Findings and Discussion
Major Results of the Study
Research has consistently shown that abnormal TSH levels can lead to significant health repercussions. Low TSH often signals hyperthyroidism, where the thyroid produces excess hormones. On the flip side, high TSH levels can indicate hypothyroidism, where the thyroid is underactive. Both conditions can lead to various symptoms affecting energy, weight, and emotional well-being.
Detailed Analysis of Findings
- Factors Influencing TSH Levels
- Implications of Abnormal Results
- Age: TSH levels tend to rise with age; thus, older adults may still fall within the normal range even if their levels are higher.
- Pregnancy: Pregnancy alters metabolism and hormone production, necessitating tailored TSH reference ranges for expectant mothers.
- Medications: Certain medications, especially those affecting thyroid hormones, can skew TSH results.
- For Hyperthyroidism: Symptoms can include weight loss, increased heart rate, and anxiety.
- For Hypothyroidism: Look out for fatigue, depression, and weight gain.
Elevated or decreased TSH levels can dramatically affect quality of life, making timely diagnosis and treatment imperative.
Understanding TSH levels is not just for endocrinologists. For students, researchers, and professionals working across health sectors, this knowledge is invaluable. By comprehensively grasping what influences TSH and recognizing the signs of its imbalance, one can advocate for proactive health measures and informed patient care.
Thus, as we endeavor to deepen our understanding of TSH, we pave the way for better individual health management and broader public health awareness.
Foreword to TSH
Understanding thyroid-stimulating hormone (TSH) is critical for anyone delving into the complexities of thyroid health. TSH is not just another hormone; it acts as a maestro, directing the symphony of thyroid hormones that help regulate metabolism, growth, and energy levels in our bodies. This section is essential because it lays the groundwork for comprehending how TSH operates and why maintaining its levels within the normal range is vital for overall well-being.
Defining Thyroid-Stimulating Hormone
At its core, thyroid-stimulating hormone is produced by the pituitary gland, which is located at the base of the brain. Its primary function is to stimulate the thyroid gland, prompting it to produce crucial hormones such as thyroxine (T4) and triiodothyronine (T3). You might think of TSH as a flickering light switch—it sends signals that tell the thyroid when to turn on production and, just as importantly, when to dial it back.
In simple terms, TSH levels can indicate how well the thyroid is functioning. When TSH is elevated, it usually signifies that the thyroid is underactive (hypothyroidism), while low TSH levels may point to an overactive thyroid (hyperthyroidism). Therefore, understanding TSH is paramount for diagnosing and managing thyroid-related ailments.
Importance of TSH in Thyroid Function
The significance of TSH extends far beyond mere hormone levels; it serves as a barometer for thyroid health. The interplay between TSH, T3, and T4 is delicate and necessary for numerous bodily functions.
Here are a few key points to consider regarding the role of TSH:
- Hormonal Balance: When TSH levels are within the normal range, the body operates in harmony, with energy production and metabolic processes functioning properly.
- Diagnostic Tool: TSH testing is a first-line diagnostic tool for identifying thyroid dysfunction. It’s often the initial test doctors will rely on when you present with symptoms like fatigue, weight changes, or mood fluctuations.
- Indicator for Other Conditions: Variations in TSH can also serve as a clue for other health issues. For example, high TSH levels might hint at a pituitary disorder or even certain types of tumors, prompting further investigation.
"A well-functioning thyroid is pivotal for overall health; without proper TSH regulation, the body’s intricate processes can go awry."
In summary, grasping the significance of TSH not only informs us about thyroid function but also offers insights into broader health issues. For everyone from students to healthcare professionals, a thorough knowledge of this hormone lays a solid foundation for diving deeper into the subject of thyroid health.
Normal TSH Range: What to Expect
Understanding the normal range of TSH levels is crucial for anyone navigating the complexities of thyroid health. Thyroid-stimulating hormone, as previously defined, is a key player in regulating thyroid function, which in turn affects a wide range of bodily processes, including metabolism, growth, and energy levels. Having a grasp on what constitutes a normal TSH level prepares individuals to interpret their health more effectively, understand the potential implications of abnormal readings, and engage in meaningful discussions with healthcare professionals.
The usual reference range for TSH is generally between 0.4 and 4.0 milliunits per liter (mU/L), yet this can fluctuate based on various factors like age, health conditions, and even geographical location. Recognizing these fluctuations is essential. Having a solid understanding of these nuances helps individuals and healthcare providers alike make informed decisions regarding diagnosis and treatment.
General Reference Values
When we speak about general reference values for TSH, it's important to recognize that these values are not set in stone. They can change based on the latest research and guidelines put forth by healthcare organizations. For most healthy adults, the TSH level should ideally be within the range of 0.4 to 4.0 mU/L. For some contexts, levels closer to 2.5 mU/L are sometimes considered optimal for a quicker identification of potential issues.
- Infants: For newborns, the normal range can be a bit more liberal, often cited as 1.0 to 15.0 mU/L, reflecting the rapid changes in hormonal activity during this developmental phase.
- Children and Adolescents: As children grow, their TSH levels typically fall within a range similar to adults, although slightly higher levels within 0.5 to 6.0 mU/L can be acceptable depending on individual growth patterns.
- Pregnant Women: During pregnancy, TSH levels can vary significantly. Generally, a lower threshold is accepted, from about 0.1 to 3.0 mU/L in the first trimester, as biological changes influence hormone levels.
Understanding these reference values helps create a baseline that can be used for further screening and diagnostics.
Variability Among Different Populations
Not all individuals are cut from the same cloth, and this holds particularly true regarding TSH levels. Variability in the normal range of TSH can be attributed to several factors, including ethnicity, geographic region, and overall health status.

- Ethnic Differences: Research has shown that populations might show different median TSH levels. For instance, some studies suggest that certain ethnic groups may experience shifts in their normative ranges due to genetic factors—meaning what's normal for one group might not apply universally.
- Geographic Influence: Environmental factors, including iodine nutrition, also come into play. People living in areas with iodine-rich diets may show different TSH levels compared to those in regions where iodine deficiency is rampant.
- Socioeconomic Status: Access to healthcare and education can affect general health literacy and awareness about thyroid health, leading to different levels of TSH testing and interpretation in distinct socioeconomic groups.
The take-home message is that no single normal TSH range fits all, and clinicians should consider these variabilities in context when evaluating a patient's thyroid health.
"Recognizing the broader context of TSH levels allows for a more personalized approach to health care, focusing on the individual rather than basing decisions solely on generalized data."
In summary, understanding the general reference values and the variabilities among different populations provides a richer, more contextual interpretation of TSH levels, enhancing overall comprehension of thyroid health.
Factors Influencing TSH Levels
Understanding the factors that influence TSH levels is vital for anyone delving into thyroid health. The thyroid-stimulating hormone is not an isolated entity; instead, it interacts with a myriad of elements in our body and environment. Getting a grasp on these influencing factors aids both clinicians and laypeople in interpreting test results more accurately, adjusting treatment plans, and fostering healthier lifestyles.
A comprehensive analysis of TSH levels must account for varying physiological and external contributors. From demographic aspects like age and gender to lifestyle choices and medication impacts, appreciating these factors enriches the conversation around TSH and thyroid function. Often overlooked, these nuances can drastically affect someone’s health outcomes and understanding, making it essential to highlight them in any thorough discussion.
Age and Gender Disparities
Age and gender exert a noteworthy influence on TSH levels. As one ages, the thyroid's performance can decline, resulting in elevated TSH levels. Interestingly, men and women experience differing norms. Women typically have higher TSH values than men throughout their lifespan. This disparity stems from hormonal fluctuations, particularly around puberty and menopause.
- Age Considerations:
- Gender Differences:
- In younger adults, TSH levels generally fall within a specific range.
- Older adults may exhibit TSH levels that indicate hypothyroidism without corresponding symptoms, complicating diagnoses.
- Studies show that women might show changes in TSH levels post-menopause due to hormonal shifts.
- Men, however, tend to have a relatively stable range throughout life, leading to a potential oversight in evaluations as they age.
Impact of Medications
Medications can significantly skew TSH levels. Various drugs can either raise or lower hormone levels, leading to misinterpretations of thyroid function. For instance, corticosteroids can impair TSH secretion, resulting in deceptively low readings. Conversely, biotin supplements, which are popular for hair and nail health, can artificially elevate results, throwing a wrench into proper diagnostics.
It's essential to understand that:
- Some medications can have a direct impact; for example, lithium is known to induce hypothyroidism.
- Others may only have indirect effects, such as certain antidepressants that can alter metabolic rates, indirectly influencing TSH.
"Medication impacts on TSH readings can be likened to a blood pressure reading after a cup of strong coffee—it may show a false high just because of transient factors."
Lifestyle Choices and Their Effects
Lifestyle factors play a dual role in influencing TSH levels. Diet, exercise, stress management, and even sleep patterns can either contribute to optimizing thyroid function or deteriorate it.
- Diet:
- Exercise:
- Stress and Sleep Patterns:
- Iodine intake is crucial. An excess or deficiency can markedly affect thyroxine production and, in turn, TSH.
- Consuming high amounts of goitrogens (found in cruciferous vegetables) can affect thyroid function when not balanced by adequate iodine consumption.
- Regular physical activity is associated with lower TSH levels as it positively impacts metabolism and hormone regulation.
- On the flip side, over-training can cause an exaggerated stress response, indirectly leading to altered TSH readings.
- Chronic stress can elevate cortisol levels, which can then suppress TSH production.
- Sleep deprivation plays a similar role, impacting hormone levels and overall health.
Common Disorders Related to TSH Levels
Understanding the common disorders related to TSH levels is critical for comprehending the broader implications on thyroid health. TSH is often regarded as a barometer for thyroid function, and deviations from the normal range can indicate significant underlying health issues. The importance of recognizing these disorders lies in both prevention and management. Early detection of hormonal imbalances can lead to timely interventions, potentially mitigating the progression of more serious diseases.
Hypothyroidism and Its Indicators
Hypothyroidism occurs when the thyroid gland fails to produce sufficient levels of thyroid hormones. Consequently, the body experiences slower metabolic functions, often leading to weight gain, fatigue, and even depression. Common indicators of hypothyroidism include:
- Fatigue and weakness
- Cold intolerance
- Dry skin and hair
- Unexplained weight gain
- Constipation
- Slowed heart rate
In cases where TSH levels are high but the thyroid hormone levels are low, hypothyroidism is typically diagnosed. The elevated TSH arises as the pituitary gland increases hormone production in response to the thyroid’s lower output. Effectively managing hypothyroidism often requires hormone replacement therapy, such as levothyroxine, restoring the balance where necessary.
Hyperthyroidism and Diagnosis
On the opposite end of the spectrum lies hyperthyroidism, characterized by excessive thyroid hormone production. Unlike its counterpart, hyperthyroidism often leads to an acceleratd metabolism, resulting in symptoms that may seem alluring initially but are profoundly detrimental in the long term. Patients might experience:
- Weight loss despite an increased appetite
- Increased heart rate
- Nervousness or anxiety
- Heat intolerance
- Tremors in the hands or fingers
- Changes in menstrual patterns
Diagnosing hyperthyroidism typically involves assessing low TSH levels alongside elevated thyroid hormone levels. Common conditions causing hyperthyroidism include Graves’ disease, toxic adenomas, and certain medications. Treatment of hyperthyroidism may include antithyroid medications, radioactive iodine treatment, or even surgery in extreme situations, emphasizing the necessity of personalized care tailored to each individual's situation.
TSH-Related Conditions: Overview
There are various conditions that can alter TSH levels beyond hypothyroidism and hyperthyroidism. For instance, certain pituitary disorders can disrupt the hormone production process, resulting in abnormal TSH readings. In addition, health issues like thyroiditis, which is inflammation of the thyroid gland, can also skew TSH levels. Other contributors can include:
- Congenital thyroid disorders: Present at birth, affecting thyroid function from a young age.
- Hashimoto's thyroiditis: An autoimmune disorder causing the immune system to attack the thyroid, potentially leading to hypothyroidism over time.
- Thyroid cancer: While rare, it can disrupt normal TSH regulation, necessitating specialized treatment and monitoring.
"In the landscape of thyroid health, understanding the interplay between TSH levels and various disorders serves as a guide for early detection and comprehensive care, impacting everything from quality of life to long-term health outcomes."

Recognizing these conditions and their related symptoms is essential. Collaborating with healthcare professionals to address any abnormalities in TSH levels ensures that individuals receive the most appropriate course of action.
Clinical Testing for TSH Levels
Clinical testing for thyroid-stimulating hormone (TSH) serves as a vital tool in understanding thyroid health. TSH plays a unique role in the endocrine system, acting like a conductor for thyroid hormones T3 and T4, balancing energy, metabolism, and overall wellbeing. Evaluating TSH levels provides insights not only into thyroid function but also into the broader aspects of health.
A primary reason TSH testing is significant is its ability to identify potential thyroid disorders early. Regular monitoring can help catch conditions such as hyperthyroidism and hypothyroidism before they result in more severe complications.
Several standard practices surround TSH testing:
- Blood Sample Collection: Usually, a healthcare professional takes a small blood sample from a vein in your arm. This simple process doesn't require much time and is often done in outpatient settings.
- Paperwork and Preparation: Before even stepping into the clinic, it's best to ensure proper documentation. Although no special preparations typically precede this test, discussing recent medications and symptoms with your doctor can help provide context.
"Routine TSH testing not only saves time but may also save lives by enabling proactive health management."
TSH testing, although straightforward, should be taken seriously. The physiological nuances of TSH levels can provide critical contextual information as part of a larger assessment.
Understanding TSH Blood Tests
When you think about the mechanics of TSH blood tests, they operate by measuring the concentration of TSH in your bloodstream. A high TSH level typically suggests an underactive thyroid (hypothyroidism), while a low level can indicate an overactive thyroid (hyperthyroidism).
Understanding the specifics of the test is essential. Common laboratory reference ranges exist, generally falling between 0.4 to 4.0 milliunits per liter (mU/L). However, these values can vary based on numerous factors, including lab methods and patient demographics.
Interpreting Test Results
Interpreting the results of a TSH test requires careful consideration. Normally, a TSH level is just a piece of the puzzle. Your healthcare provider will often consider these results alongside symptoms and other tests. Here’s how the various levels might be perceived:
- Normal Range (0.4 - 4.0 mU/L): Indicates adequate thyroid function.
- High TSH (>4.0 mU/L): May suggest hypothyroidism or insufficient thyroid hormone production.
- Low TSH (0.4 mU/L): Often linked to hyperthyroidism, where there’s an excess of thyroid hormone in circulation.
Putting it all together, it's vital to remember that context is king when interpreting these results; they should never stand alone.
Routine Screening Recommendations
Quite a few health organizations recommend routine TSH screening under certain situations. For instance:
- Adults over 60 Years: Health providers may suggest regular annual screenings due to age-related changes in thyroid function.
- Pregnant Women: Levels should be monitored closely as thyroid function directly influences pregnancy outcomes.
- Family History of Thyroid Disease: If you have relatives with thyroid issues, getting tested might be a wise step.
Overall, engaging in regular TSH testing can ensure you're on top of your thyroid health, allowing for timely interventions when abnormalities are detected. Monitoring these levels can be pivotal in maintaining overall health.
Abnormal TSH Levels: Implications
Understanding abnormal TSH levels is key to unraveling various thyroid-related health concerns. When TSH levels stray from the norm, they can indicate underlying issues that might require further medical investigation. This section will explore low and high TSH levels, giving insight into what these irregularities signify and the possible consequences they carry.
What Low TSH Indicates
A low TSH level can signal that the body is producing too much thyroid hormone, commonly associated with hyperthyroidism. This condition can stem from several sources.
- Graves' Disease: An autoimmune disorder that stimulates the thyroid to produce excess hormones.
- Toxic Nodular Goiter: A benign growth that can lead to an overproduction of hormones.
- Excessive Iodine Intake: This might occur through dietary sources or medications.
Low TSH can bring about a range of symptoms, including:
- Rapid weight loss despite normal eating habits
- Increased heart rate or palpitations
- Anxiety or nervousness
- Heat intolerance and increased sweating
- Fatigue or muscle weakness
"Low TSH levels can open the door to a range of symptoms that can degrade one’s quality of life, and understanding these implications is pivotal for timely intervention."
Understanding High TSH Levels
Conversely, high TSH levels often indicate an underactive thyroid or hypothyroidism. This means the thyroid isn’t producing enough hormones, thus revving up the TSH production as the pituitary gland attempts to stimulate it.
Common causes of elevated TSH include:
- Hashimoto's Thyroiditis: An autoimmune disorder where the body attacks thyroid tissues.
- Certain Medications: Drugs such as lithium or amiodarone can affect thyroid hormone production.
- Thyroid Surgery or Radiation: These interventions may lead to diminished thyroid function.
Elevated TSH levels can produce symptoms like:
- Unexplained weight gain
- Fatigue and sluggishness
- Increased sensitivity to cold
- Dry skin and hair loss
- Depression or mood changes
Differential Diagnosis for TSH Anomalies
When TSH test results show abnormalities, further investigations are often warranted to identify the underlying cause. This may involve:
- Free T4 and Free T3 Testing: To directly assess the levels of active thyroid hormones in the blood.
- Thyroid Antibody Tests: To check for autoimmune conditions such as Hashimoto’s or Graves'.
- Imaging Studies: Such as ultrasound, to visualize the thyroid gland.
Differential diagnosis is essential not only to confirm the type of thyroid dysfunction but also to rule out other conditions. Some factors for consideration include:

- Patient's age and sex
- Family history of thyroid disease
- Presence of thyroid nodules or goiter
- Symptoms profile
When interpreting TSH levels, context is vital. They can provide important clues, but they should always be understood alongside other laboratory results and clinical evaluations to build a complete picture of the individual's thyroid health.
Treatment Approaches for Abnormal TSH
The significance of addressing abnormal TSH levels cannot be overstated. Given that TSH is pivotal in the regulation of thyroid function, its fluctuations can lead to considerable health implications. Management strategies can vary widely, depending on whether the TSH levels are elevated or decreased. Understanding the specific treatment options not only aids in mitigating symptoms but also helps to restore overall hormonal balance. Therefore, grappling with abnormalities in TSH gives rise to treatment modalities tailored to the individual, based on the underlying condition.
Hypothyroidism Treatment Options
When TSH levels are high, it often indicates that the body is struggling with hypothyroidism. This condition arises when the thyroid gland does not produce sufficient hormones. The primary treatment approach usually involves hormone replacement therapy.
- Levothyroxine is the most common medication used. It is a synthetic form of the thyroid hormone thyroxine (T4) and effectively normalizes TSH levels. Patient adherence to this medication is crucial, as consistent dosage ensures stable hormone levels.
- Regular monitoring of TSH levels is vital once treatment begins. This ensures that dosage adjustments can be made as needed, optimizing treatment efficacy.
- A proposed diet might also play a supportive role. Incorporating iodine-rich foods, for instance, could enhance thyroid function. However, it's essential for patients to consult healthcare providers before making significant dietary changes.
Additionally, some individuals might benefit from complementary therapies, such as:
- Selenium supplements for enhanced thyroid health.
- Stress management practices, which can indirectly influence thyroid function.
Ultimately, a multidisciplinary approach, involving healthcare providers, dietitians, and sometimes endocrinologists, ensures comprehensive management of hypothyroidism.
Management of Hyperthyroidism
Conversely, when TSH levels are low, hyperthyroidism could be the culprit. This condition results from the overproduction of thyroid hormones, leading to a plethora of symptoms like anxiety, weight loss, and heat intolerance. Managing hyperthyroidism requires a different set of strategies:
- Antithyroid medications, such as Methimazole, are frequently prescribed to inhibit hormone production by the thyroid gland.
- Radioactive iodine therapy is another viable option, particularly for patients who do not respond adequately to medication. This treatment destroys overactive thyroid cells, thus reducing hormone production over time.
- In some cases, especially when other treatments fail or if there are complications, surgical intervention may be warranted. Thyroidectomy, the surgical removal of part or all of the thyroid gland, can provide long-term relief from hyperthyroidism.
It's critical to note that hyperthyroidism can also emerge from various autoimmune disorders, such as Graves' disease. Recognizing the specific underlying cause can significantly influence the chosen treatment strategy.
Like hypothyroidism, lifestyle changes can assist in managing hyperthyroidism. Avoiding excessive iodine, reducing stressors, and maintaining a balanced diet are helpful practices. Collaborating with healthcare professionals ensures that the treatment plan is well-rounded and tailored to the individual's needs.
In both cases of abnormal TSH, regular follow-ups and assessments will help ensure that treatment remains effective and any necessary adjustments are made promptly.
Future Perspectives in TSH Research
The field of thyroid research is continuously evolving, and the future perspectives regarding TSH (Thyroid-Stimulating Hormone) are drawing attention from many healthcare professionals and researchers. Comprehending these future directions is crucial, as they not only impact how we understand thyroid health but also influence treatment protocols and diagnostic methodologies.
One significant area of focus is on the refinement of testing methods. As science advances, new technologies and techniques for measuring TSH levels are emerging. Innovative testing methods promise greater accuracy and efficiency, enabling clinicians to identify abnormalities more quickly and reliably. Enhanced testing could potentially lead to improved patient outcomes by allowing for more tailored treatment approaches.
Another element in this discourse is the exploration of individual variability in TSH levels. There is a growing recognition that one-size-fits-all reference ranges may not be sufficient. Emerging research indicates that genetic and environmental factors may influence normative ranges for different demographics. This understanding may pave the way for personalized medicine, where treatment plans are customized based on a patient’s specific needs.
"Identifying TSH variations that arise from genetic factors could transform how we approach thyroid disorders and treatment."
Moreover, with advancements in biotechnology, we may see novel therapies developed that specifically target TSH regulation. These initiatives could hold the key to not only managing hypothyroidism and hyperthyroidism but also other TSH-related conditions, such as autoimmune diseases affecting the thyroid. This presents a hopeful horizon where patients may benefit from innovative treatments that tackle the root of their issues instead of merely alleviating symptoms.
Innovative Testing Methods
New testing methodologies are on the horizon that aim to make TSH measurements more nuanced. With rising demand for precision in healthcare, researchers are looking into not just blood tests but also alternative mediums for testing. Salivary and urinary tests might prove valuable, as they can offer less invasive options with a broader view of hormone levels over time. This is especially promising for patients who might find regular blood draws cumbersome.
- Point-of-care Testing: Technologies that allow TSH testing in a clinical setting at the moment of consultation. This offers immediate feedback and can expedite decision-making processes regarding treatment.
- Wearable Technology: Devices that measure hormone levels in real-time could also emerge, giving individuals continuous insight into their thyroid health. This would advance proactive healthcare, shifting from reactive strategies to prevention-focused approaches.
Potential Developments in Treatment
As we look to the future, potential developments in treatment for thyroid disorders associated with abnormal TSH levels are promising. Research efforts are peering into better pharmaceutical options and novel biological therapies that could redefine existing paradigms. These efforts include:
- Targeted Therapies: Focused on modifying TSH levels directly, thus providing a more targeted means of either reducing TSH in cases of hyperthyroidism or elevating it in cases of hypothyroidism with fewer side effects.
- Biologics: The development of biologics is expected to engage the immune response more effectively. They could intervene in autoimmune thyroiditis, a condition that leads to altered TSH levels, significantly improving patient care outcomes.
- Gene Therapy: Advancements in gene therapy might eventually pave the way for altering the expression of thyroid function-related genes, addressing the root of TSH imbalances rather than just their symptoms.
As these developments emerge, they may require alterations to existing guidelines and practices around TSH management. Thus, ongoing education for healthcare providers will be essential to keep abreast of these advancements, ensuring that patients benefit from cutting-edge solutions.
End
The conclusion serves as a linchpin in our exploration of TSH and its normal range, solidifying the knowledge acquired throughout this comprehensive review. Understanding TSH levels is not merely academic; it has real-world implications for health and well-being. TSH, as a crucial hormone for regulating thyroid function, directly influences diverse bodily functions, such as metabolism and energy levels. Therefore, maintaining TSH within the normal range is essential for optimal health.
"Monitoring TSH levels can provide significant insights into a person's thyroid health, impacting decisions regarding treatment and lifestyle adaptations."
Summary of Key Points
In revisiting the essential points discussed in this article, it’s clear that:
- The normal range for TSH levels typically hovers between 0.4 to 4.0 mIU/L, although individual variance can occur based on multiple factors.
- Factors like age, gender, medications, and lifestyle choices can significantly impact TSH levels, creating a need for personalized assessments.
- Abnormal TSH levels indicate potential thyroid issues, with hypothyroidism characterized by elevated TSH and hyperthyroidism by reduced TSH.
- Advances in clinical testing for TSH levels enhance the ability to diagnose and treat thyroid-related conditions efficiently.
Recognizing these key aspects lays a strong foundation for understanding not just TSH itself but also its wider implications in health.
Final Thoughts on TSH and Health
Considering TSH levels in a broader context emphasizes their significance well beyond clinical parameters. They can be viewed as a barometer for whole-body health. Regular monitoring can lead to early detection of thyroid disorders, which is crucial for initiating timely interventions. This is particularly important in populations at risk for thyroid dysfunction, such as pregnant women and those with a family history of thyroid issues.
In essence, the journey of understanding TSH levels is deeply intertwined with individual health narratives. Anyone invested in their health should consider this hormone's implications seriously. Armed with the right information, they can advocate for their health proactively, making informed choices about their well-being.
Engaging with healthcare providers about TSH tests and understanding the results can empower individuals to take control of their health. Ultimately, the knowledge of TSH levels isn't just about numbers; it's about health, vitality, and informed living.







